Mechanical ventilation and ICU ventilators are critical components in the management of patients with severe respiratory conditions. Understanding their functionality and application is essential for effective patient care. These technologies play an important role in supporting and stabilizing patients in critical conditions.
What is Ventilation?
ICU Ventilation is the process of movement of air from the atmosphere through the airways to the terminal respiratory gas exchange units by the effort of the respiratory muscles or mechanical ICU ventilators if the patient is being ventilated.
What is Respiration?
Oxygen is essential for life. It is required by each human cell for its survival. It is abundantly present in the atmosphere and maintains a remarkably constant concentration of 20.9% in ambient air. Oxygen is taken up by the lungs through the act of inspiration and transported to the cells via the blood.
At the cellular level, oxygen is utilized for the production of energy. In this process, carbon dioxide is released and transported back via the blood to the lungs from where it is expired out into the atmosphere. The act of the exchange of oxygen and carbon dioxide is called respiration.
What is the Difference Between ICU Ventilators and Respirator?
A ventilator is a machine, a system using mechanical power and having several parts, each with a definite function and together performing a particular task. The task here is to provide all or part of the body’s work that is called breathing or ventilation. Respirator is an apparatus that people worn it over their mouth and nose or the entire face to prevent the inhalation of dangerous substances such as: dust, smoke, etc
Indications for Ventilation
Patients who require ventilatory support often develop a common pattern of physiological deterioration, including:
- changes in respiratory rate
- asynchronous respiratory pattern
- changes in mental status and changes in level of consciousness
- frequent oxygen desaturation despite increasing oxygen concentration
- hypercapnia and respiratory acidosis
- circulatory problems, including tachypnea, tachycardia, hypertension, or hypotension.(3)
What is Non-invasive Ventilation (NIV)?
NIV refers to the provision of respiratory support without direct tracheal intubation. As such, it aims to avoid some of the complications inherent with invasive ventilation, such as the need for sedation with risks of hemodynamic instability and subsequent risk of delirium, nosocomial infection, etc.(2)
Recommendations for the use of non-invasive ventilation(4):
- COPD exacerbations
- Facilitation of weaning/extubation in patients with COPD
- Cardiogenic pulmonary edema
- Immunosuppressed patients
- Do-not-intubate status
- End-stage patients as palliative measure
- Extubation failure (COPD or congestive heart failure) (prevention)
- Community-acquired pneumonia in COPD
- Postoperative respiratory failure (prevention and treatment)
- Prevention of acute respiratory failure in asthma
Goals of Mechanical Ventilation
One of the most important treads of life support in the emergency department is Mechanical ventilation (MV). It provides time for recovery until the patient’s physiological balance is restored. This is why MV alone is not a unique and specific treatment for a particular disease; however, it has two general and main purposes: to support the injured lung and to protect the healthy lung.
Specific Goals of Mechanical Ventilation
- Reversal of Apnea
- Reversal of Respiratory Distress
- Reversal of Severe Hypoxemia
- Reversal of Severe Hypercapnia
- Goals of Mechanical Ventilation in Postoperative
- Respiratory Failure and Trauma
- Goals of Mechanical Ventilation in Shock
One of the specific goals of MV is to promote the optimization of arterial blood gas levels and acid-base balance by providing oxygen and eliminating carbon dioxide (ventilation).(1) For patients with chronic diseases MV can reduce the work of breathing by taking effort from respiratory muscles and maintaining long-term respiratory support.
The ventilator is not a magical therapy that makes patients better but simply a supportive therapy used until more definitive therapies have time to work.
Apnea
Patients with apnea, such as those who have suffered catastrophic central nervous system (CNS) damage, need the immediate institution of mechanical ventilation.(2)
Indications and Contraindications for Non-invasive Ventilation
Recognizing when and when not to use NIV is crucial for its effective application. Below, we have explained the indications and contraindications for non-invasive ventilation for you
Indications (3)
- Moderate to severe dyspnoea
- Tachypnoea (>25–30 breaths/minute)
- Signs of increased work of breathing (abdominal paradox; accessory muscle use)
- Fatigue
- Acute-on-chronic respiratory failure: pH <7.35; pCO2 >6
- Hypoxaemia (use with caution): paO2/FiO2 <27 Kpa
Contraindications (3)
- Facial burns/trauma/recent facial upper airway surgery
- Vomiting
- Upper gastrointestinal surgery
- Copious respiratory secretions
- Severe hypoxemia
- Hemodynamically instability
- Severe co-morbidities
- Confusion/agitation
- Low Glasgow coma score
- Unable to protect the airway
- Bowel obstruction
- Respiratory arrest
NIV today consists almost exclusively of the delivery of positive pressure ventilation via an external interface. There are six broad types of interfaces available;
- total face masks (enclose mouth, nose, eyes)
- full-face masks (enclose mouth and nose)
- nasal mask (covers nose but not mouth)
- mouthpieces (placed between lips and held in place by lip seal)
- nasal pillows or plugs (inserted into nostrils)
- helmet (covers the whole head/all or part of the neck – no contact with face).(3)
What is Invasive Ventilation?
Invasive mechanical ventilation requires access to the trachea, most commonly via an endotracheal tube, and represents the commonest reason for admission to the ICU.(5)ICU Ventilators.
Large multinational surveys confirm the common indications for invasive ventilation to be:
- coma 16%
- COPD 13%
- ARDS 11%
- heart failure 11%
- pneumonia 11%
- sepsis 11%
- trauma 11%
- postoperative complications 11%
- neuromuscular disorders 5%.
- NIV contraindications.(5)
Let’s Meet with Biyovent ICU Type Mechanical Ventilator
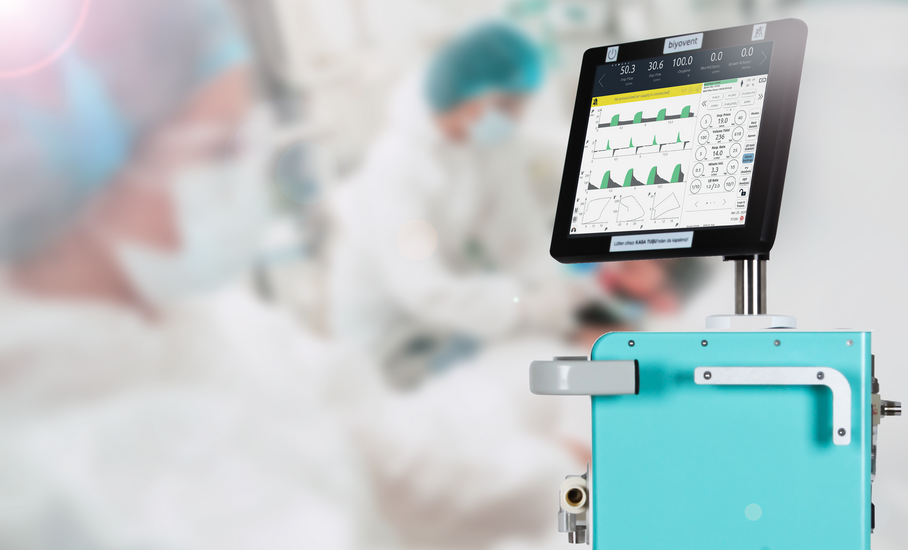
Biyovent ICU Type Mechanical Ventilator
ICU Ventilator of Biyovent makes a difference in the ventilation process with its unique specifications. Biyovent has been carefully thought out with every detail of the ventilators and developed with a holistic approach. Prepared for mass production in cooperation with Arçelik, Baykar, and Aselsan. ICU Ventilators
What are some specific features of Biyovent?
⦁ Invasive and Non-invasive Ventilation
⦁ Integrated Nebulizer
⦁ High Flow Oxygen Therapy
⦁ Suitable for Pediatric, Adult and Newborn (Optional) Patients
⦁ Smart Ventilation Modes
Learn more details about Biyovent ICU Ventilator
Get in contact with the Biosys Sales Team
References
1- Frank Lodeserto MD, “Simplifying Mechanical Ventilation – Part I: Types of Breaths”, REBEL EM blog, March 8, 2018. Available at: https://rebelem.com/simplifying-mechanical-ventilation-part/.
2- Tobin M.J. 3rd edn. McGraw-Hill Education; 2012. Principles and practice of mechanical ventilation.
3- Popat B, Jones AT. Invasive and non-invasive mechanical ventilation. Medicine (Abingdon). 2012;40(6):298-304. doi:10.1016/j.mpmed.2012.03.010
4- Hess D.R. The evidence for noninvasive positive-pressure ventilation in the care of patients in acute respiratory failure: a systematic review of the literature. Respir Care. 2004;49:810–829.
5- Esteban A., Ferguson N.D., Meade M.O. Evolution of mechanical ventilation in response to clinical research. Am J Respir Crit Care Med. 2008;177:170–177

